How Zero Flow can Trigger Graft Revision in LIMA-Cx Grafts
The following two cases demonstrate how critical flow measurement is in determining the patency of a bypass graft. The bypass grafts in each of the cases first measured 0 ml/min flow. Flow improved appreciably after revision of the grafts.
Case No. 1
A 78-year-old female patient underwent single coronary bypass grafting to bypass a blocked circumflex (Cx) coronary artery with the LIMA bypass graft. Following anastomosis of the LIMA to the Cx distal to the blockage, flow measured 0 mL/min (PI: 91). The flow waveform had a spiky systolic profile (top waveform). Revision was demanded.
Following revision of the graft, mean graft flow improved to 32 mL/min (PI: 2), and the waveform exhibited a balanced systolic/diastolic profile (bottom waveform). Zero mean flow was the determining factor in the decision to revise the graft.
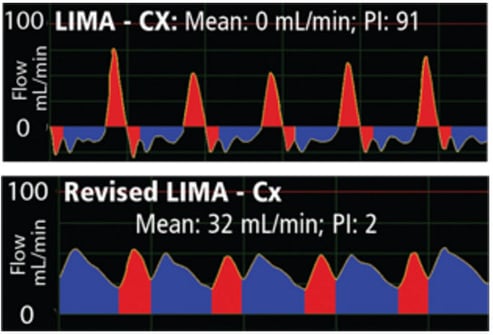
The top waveform exhibited a spiky systolic profile, which, accompanied by zero mean flow, called for the surgeon to revise the LIMA-Cx graft without hesitation. Flow improved to 32 mL/min after revision and the waveform exhibited a balanced LIMA-Cx profile (bottom waveform).
Case No. 2
A 78-year-old male patient underwent OPCAB. The LIMA was used as a bypass to the Cx. Initial flow measured 0 mL/min and was accompanied with a systolic waveform profile.
The graft was revised and flow increased to 32 mL/min. Flow exhibited a more balanced systolic/diastolic waveform (lower waveform). The PI went from 100 to 2.
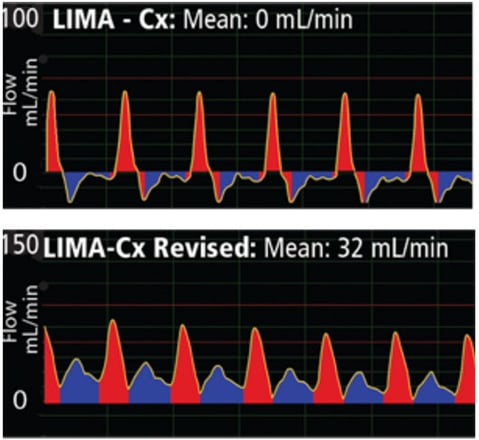
The upper spiky systolic waveform profile shows initial 0 mL/min LIMA-Cx graft flow following anastomosis of the bypass. After the graft was revised, flow increased to 32 mL/min and was accompanied by a more balanced diastolic/systolic profile (lower waveform).




