Zero Vascular Access Recirculation — the New Reality
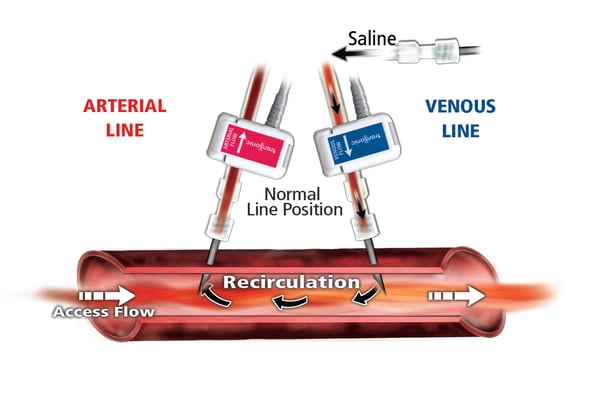
Access recirculation occurs when a portion of the blood returning from the dialyzer recirculates though the arterial line rather than passing through the venous circuit. Recirculation generally occurs when access flow (AF) is less than dialysis pump flow (Qb). Underdialysis occurs when recirculation is present and recirculation is now considered a late indicator of a failing access.
Traditional methods such as blood urea nitrogen (BUN) sampling can not separate recirculation of dialyzed blood through the access from recirculation through the cardiopulmonary system (cardiopulmonary recirculation or CPR). Therefore, recirculation was often overestimated. Modalities that cannot separate cardio-pulmonary recirculation from access recirculation will indicate false positive recirculation. On the other hand, Transonic ultrasound dilution technology is able to separate actual peripheral vascular access recirculation from cardiopulmonary recirculation. Consequently, measurement of zero percent access recirculation became the new recirculation standard.
Causes of Recirculation
When a venous stenosis occurs, and access flow does not meet pump demands, some newly dialyzed blood from the venous line recirculates immediately back into the arterial line to compensate for a flow deficit at the arterial needle. Although access recirculation generally occurs when access flow is less than dialysis pump flow, an important exception exists when a stenosis occurs between the dialysis needles. Because the stenosis limits flow through the access, the pump simply bypasses the stenosis altogether and zero recirculation is reported. Finally, if surveillance detects vascular access recirculation but the recirculation disappears after the blood lines are reversed, the hemodialysis lines have been inadvertently reversed and there is no true recirculation.
MacDonald JT et al, ”Identifying a New Reality: Zero Vascular Access Recirculation Using Ultrasound Dilution,” ANNA J 1996; 23(6): 603-8.



