Transonic Flowmeters Used in Development of Extra-Uterine Womb
 Over a third of infant deaths and half of cerebral palsy diagnoses in the United States are attributed to premature birth. Despite advances in neonatal intensive care that have increased the limits of viability, survivors of premature birth before 28 weeks often deal with chronic lung disease and other complications from immature organs.
Over a third of infant deaths and half of cerebral palsy diagnoses in the United States are attributed to premature birth. Despite advances in neonatal intensive care that have increased the limits of viability, survivors of premature birth before 28 weeks often deal with chronic lung disease and other complications from immature organs.
Bronchopulmonary dysplasia — an arrest in lung development secondary to premature transition from liquid to gas ventilation — is the most common and challenging problem facing extremely premature infants.
In an effort to create a more physiological approach to support these infants, researchers at Children’s Hospital of Philadelphia (CHOP) created an extra-uterine womb.
How it Works
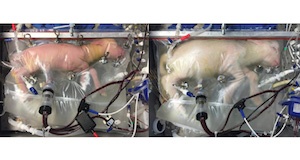
Researchers delivered premature lambs and placed them into a sterile bag filled with electrolyte fluid. Then, tubes carrying oxygenated blood were plugged into the lamb’s umbilical cord. This allows the lamb’s heart to pump blood at volumes and pressure comparable to what a placenta would provide. The fluid inside the artificial womb helps the lamb’s lungs develop as they would while still in utero.
In order for the extra-uterine womb to be used on human infants, the babies would have to be born surgically and placed into the fluid incubator. This presents an issue, says lead researcher Alan Flake, because up to 50 percent of extremely premature infants are born vaginally. Also, delicate fetal surgery would need to be performed to connect the baby’s umbilical cord to the ventilator while he or she is still attached to his or her mother.
However, Flake and his team estimate that once these and other issues are corrected, the device may be ready for human trials in as little as five years.
Transonic’s Flowmeters Used
According to the report published in Nature Communications, “Connections were established as an arterial-venous extracorporeal oxygenation circuit, with the carotid artery or umbilical arteries providing inflow to the oxygenator (CA/JV or UA/UV) connected to the oxygenator inflow port and the jugular vein or umbilical vein (CA/JV or UA/UV) providing outflow from the oxygenator and connected to the oxygenator outflow port.”
Researchers used Transonic’s HXL Tubing Flowsensor to continuously measure circuit flow. Researchers also used the HXL Tubing Flowsensor to monitor the level of fluid volume in the artificial amniotic sac.
“It was such a thrill to scroll through the news and see Transonic Flowmeters being used in this groundbreaking research on the development of an extra-uterine womb to support premature fetal development,” said Margo Sosa, Senior Research Product Manager at Transonic. “As a company whose roots began in research over 30 years ago, Transonic has tremendous pride in seeing our products used to support the type of truly revolutionary science that Dr. Flake and his team at CHOP are working on. Being able to be even a small part of something like this is the kind of kick that makes us excited to get up and go to work every morning!”
Image source: E.A. PARTRIDGE ET AL/NATURE COMMUNICATIONS 2017




